The Clean, Green Everything Store on a Mission.
Explore 500+ Eco-Friendly, Sustainable and Organic Brands. Learn More
Discover Our Broad Spectrum of Choices
Why Choose Love?
-
Commerce with a Purpose
Shop from 500+ eco-conscious, sustainable brands, enjoying unbeatable prices and a diverse selection.
Free Shipping: On orders over $49.99, with order tracking and timely updates on your order status.
Fast, Secure Checkout: Available guest-checkout, backed by secure transactions and trusted payment methods.
Hassle-Free Returns: Easy 30-day return policy, ensuring stress-free refunds and returns. -
Mission-Driven Marketplace
Discover where health, sustainability, and innovation merge. We continuously scout the country for top-quality, eco-aligned brands, adding new selections weekly. From startups to established names, our brands are united in eco-consciousness.
Find groundbreaking wellness products, healthy snacks, herbal tonics, and sustainable home essentials, all chosen for the environmentally-aware shopper.Explore our evolving range and embrace the latest in sustainable living. Learn More
-
Giving Back 20% Pledge
Dedication to Giving Back: Love.com commits 20% portion of our net profits to local communities. We select non-profits that align with our Love Standards, focusing on excellence and meaningful impact.
We welcome this framework to all companies, not just our own, to embrace corporate giving in a serious way.
Our community initiatives and partnerships are an integral part of this mission. Learn More.
Currently Trending
Explore Our Top-Selling Products.
-
Oxalis Triangularis Purple False Shamrock by Bumble Plants
Brand:Bumble Plants3.0 / 5.0
(0) 0 total reviews
Regular price $28.40Regular priceUnit price / per$26.00Sale price $28.40 -
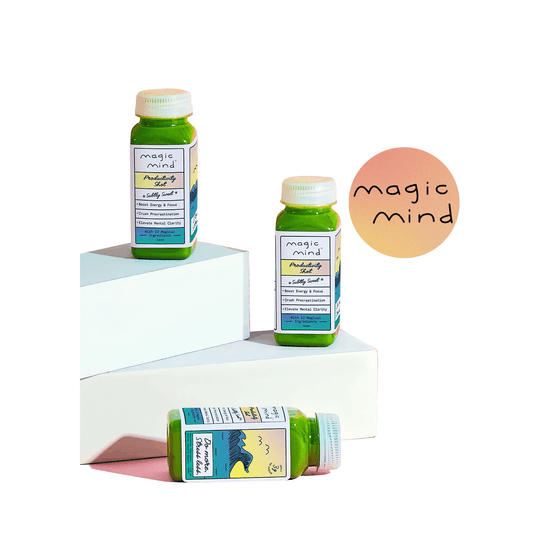
Magic Mind Productivity Shot with Nootropics and Adaptogens by Magic Mind
Brand:Magic MindRegular price From $89.25Regular priceUnit price / per -
Certified Organic Palo Azul Tea By MagikTea, 15 Loose Tea Bags, The Alkaline Florescent Herbal Tea High in Polyphenols
Brand:MagikteaRegular price $13.99Regular priceUnit price / per -
Organic Liver Detox Drink | The Plug Drink by The Plug Drink
Brand:The Plug DrinkRegular price From $14.99Regular priceUnit price / per$14.99Sale price From $14.99 -
Magnesium Mist Chloride by Come Alive Naturals, 236 ml. Bottle
Brand:Come Alive Herbals5.0 / 5.0
(0) 0 total reviews
Regular price $40.00Regular priceUnit price / per -
Shampoo & Conditioner Set for Hair Growth, Moisture, and Shine by The Earthling Co.
Brand:The Earthling Co.4.67 / 5.0
(1) 1 total reviews
Regular price $31.98Regular priceUnit price / per$31.98Sale price $31.98 -
String of Pearls by Bumble Plants
Brand:Bumble PlantsRegular price From $22.04Regular priceUnit price / per$52.00Sale price From $22.04Sale -
Ground Beef Freeze Dried - #10 Can by Nutristore
Brand:NutristoreRegular price From $69.99Regular priceUnit price / per$69.99Sale price From $69.99 -
Sunstone - Herbal Yoga Mat by okoliving
Brand:okolivingRegular price $188.00Regular priceUnit price / per -
Non-Alcoholic Whiskey Alternative by Ritual Zero Proof
Brand:Ritual Zero ProofRegular price $29.99Regular priceUnit price / per$32.95Sale price $29.99Sale -
Reusable Pour Over Coffee Filter for Chemex and Hario V60 (Copper) by Barista Warrior
Brand:Barista WarriorRegular price $34.99Regular priceUnit price / per$50.00Sale price $34.99Sale -
Charcoal Detoxifying Body Wash Bar by KITSCH
Brand:KITSCHRegular price $10.00Regular priceUnit price / per$10.00Sale price $10.00
Highly unique and curated health articles.
-

Probiotic Multi Enzyme Supplements: Your Guide ...
Introduction to Probiotic Multi Enzyme Supplements Our bodies are incredible machines, capable of orchestrating complex processes, including digestion. Central to this are the friendly bacteria known as probiotics and the...
Probiotic Multi Enzyme Supplements: Your Guide ...
Introduction to Probiotic Multi Enzyme Supplements Our bodies are incredible machines, capable of orchestrating complex processes, including digestion. Central to this are the friendly bacteria known as probiotics and the...
-

From Farm to Table: The Sustainable Journey of ...
Supporting Local Agriculture: A Path to SustainabilityAt Love.com, we believe in the power of supporting local agriculture as a way to build a more sustainable food system. By choosing farm-to-table...
From Farm to Table: The Sustainable Journey of ...
Supporting Local Agriculture: A Path to SustainabilityAt Love.com, we believe in the power of supporting local agriculture as a way to build a more sustainable food system. By choosing farm-to-table...
-

Unlocking Productivity: The Benefits of a Heigh...
Introduction: Embracing Productivity and Well-being Through Height-Adjustable Standing DesksWelcome to Love.com, where we believe in unlocking your full potential by providing you with innovative and sustainable solutions for your everyday...
Unlocking Productivity: The Benefits of a Heigh...
Introduction: Embracing Productivity and Well-being Through Height-Adjustable Standing DesksWelcome to Love.com, where we believe in unlocking your full potential by providing you with innovative and sustainable solutions for your everyday...